Forms and Reports
The EDI 837P (Professional) is the standard format used by health care professionals and suppliers to transmit health care claims electronically. The Form CMS-1500 is the standard paper claim form to bill Medicare Fee-For-Service (FFS) Contractors when a paper claim is allowed. While the forms differ on their modes, both of them are usually suitable for billing various government institutions and several private insurers. Apart from Medicare carriers, these forms may be billed to durable medical equipment provider for waiving electronic claims.
The HIPAA (Health Insurance Portability and Accountability Act) Eligibility Transaction System (HETS) allows you to check Medicare beneficiary eligibility data in real-time. Use HETS to prepare accurate Medicare claims, determine beneficiary liability, or check eligibility for specific services.
The Explanation of Benefits (EOB) provides details about a Medicare claim that has been processed and explains based on your Medicare beneficiary eligibility what portion was paid to the health care provider and what portion of the payment, if any, is the patient's responsibility. The EOB is not a bill. Any portion of the medical expense not covered by Medicare, such as a deductible or a co-pay, will be billed by the provider and should be paid directly to the provider.
Medicare Informatics provides a solution that harmoniously integrates the above components to form a subsystem and the application as a whole.
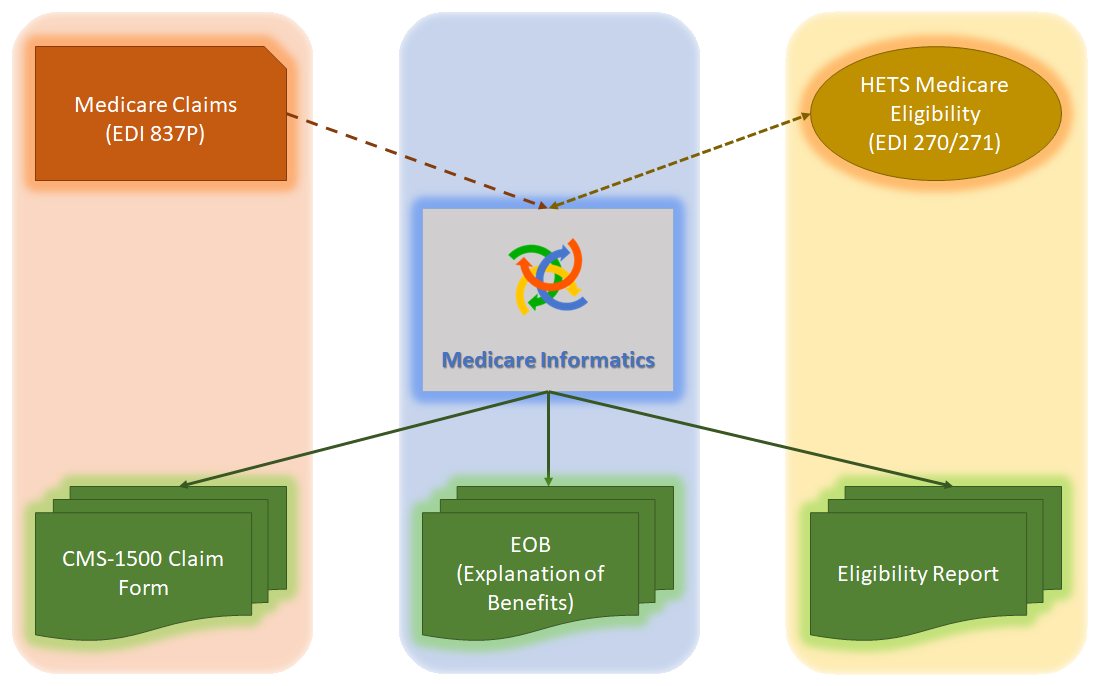
Convert an EDI 837P File transaction into CMS-1500 PDF Forms
Inquiry and Report Medicare beneficiary eligibility
Report the health care provider and the patient's payment