Merit-based Incentive Payment System (MIPS)
Medical providers are now paying more of their attention to managing patients through the entire care journey, because providers' earnings are compensated for healthy outcomes rather than each service provided.
The Quality Payment Program (QPP) takes a comprehensive approach to payment. Instead of basing payment only on a series of billing codes, the Quality Payment Program adds consideration of quality through a set of evidenced-based measures that were primarily developed by clinicians. The program recognizes and encourages improvements in clinical practice. All of these efforts are increasingly supported by advances in technology that allow for the easy exchange of needed information while protecting patient privacy. The program provides special provisions for those participating in certain new models of care that provide an alternative to fee-for-service.
Under Merit-based Incentive Payment System (MIPS), Physician Quality Reporting System (PQRS), theValue-Based Modifier (VB) program, and the Meaningful Use (MU) Medicare incentive program will be consolidated into one program and they provide clinicians flexibility to choose the activities and measures that are most meaningful to their practice to demonstrate performance.

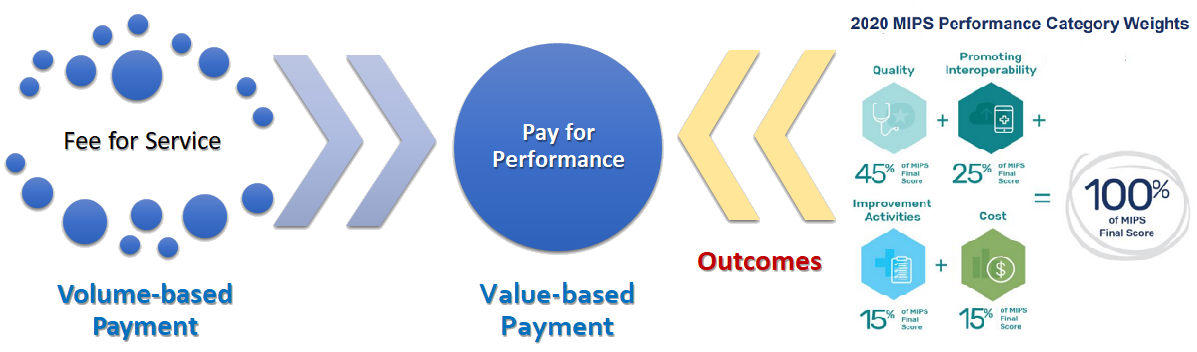
2020 MIPS Performance Categories
Quality (45%) |
Replaces Physician Quality Reporting System (PQRS).
This category covers the quality of the care you deliver, based on performance measures created by CMS, as well as medical professional and stakeholder groups.
At least 6 measures; 1 must be: Outcome or High-priority measure in the absence of an applicable outcome measure, or a complete specialty measure set.
Promoting Interoperability (25%) |
Replaces the Medicare EHR Incentive Program (also known as Medicare Meaningful Use).
CMS is re-naming the Advancing Care Information performance category to Promoting Interoperability (PI) to focus on patient engagement and the electronic exchange of health information using certified electronic health record technology (CEHRT).
Not having a 2015 Certified EHR will limit your ability to pick the best 90-days.
Improvement Activities (15%) |
Attest to participation in activities that improve clinical practice.
Includes an inventory of activities that assess how you improve your care processes, enhance patient engagement in care, and increase access to care. The inventory allows you choose the activities appropriate to your practice from categories such as, enhancing care coordination, patient and clinician shared decision-making, and expansion of practice access.
Cost (15%) |
Replaces the Value-Based Payment Modifier (VM or VBM) and helps create efficiencies in Medicare spending.
The cost of the care you provide will be calculated by CMS based on your Medicare claims.
CMS will evaluate performance on two measures (Medicare Spending per Beneficiary and Total Per Capita Cost) and the 18 episode-based measures.
