Value-Based Care
Value-based care is a form of reimbursement (with incentive payment) that ties payments for care delivery to the quality of care provided with Medicare and rewards providers for both efficiency and effectiveness. This form of reimbursement has emerged as an alternative and potential replacement for fee-for-service reimbursement which pays providers retrospectively for services delivered based on bill charges or annual fee schedules.
It is the part of CMS’s larger quality strategy to reform how health care is delivered and paid for and it also aims to advance the triple aim of providing better care for individuals, improving population health management strategies, and reducing healthcare costs.

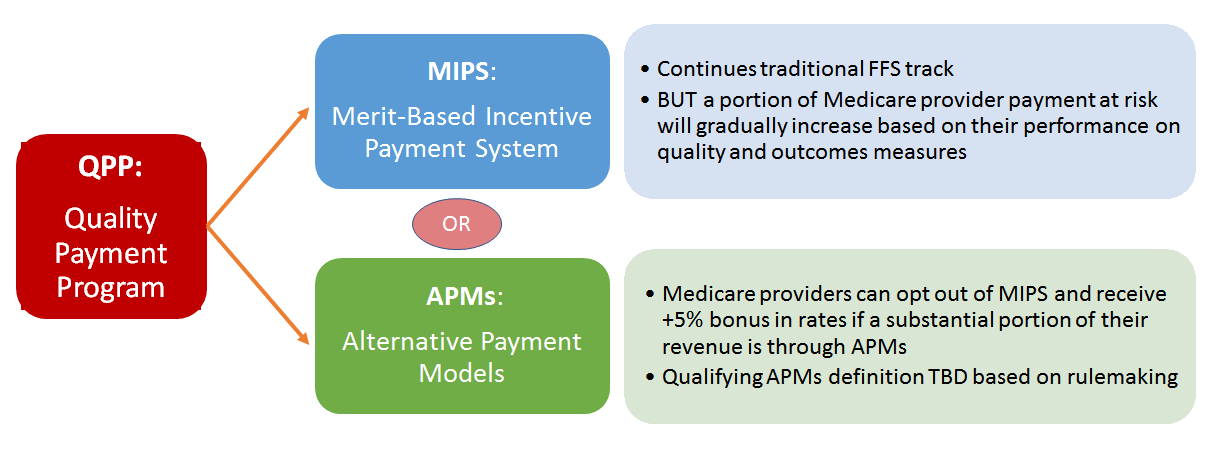
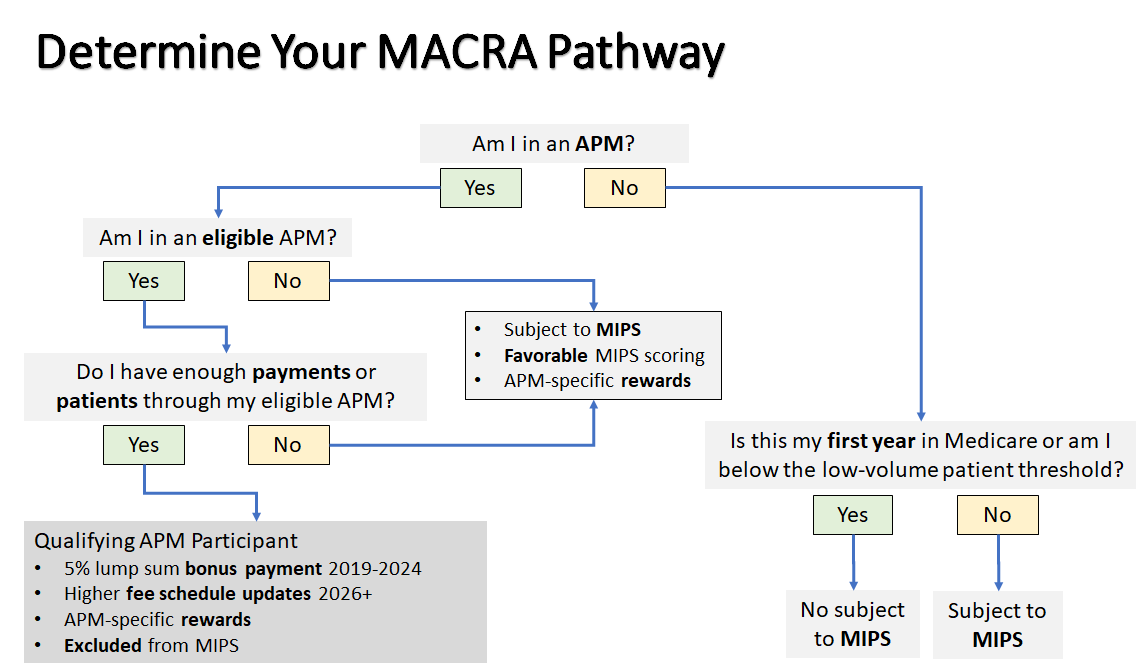
The CMS Quality Payment Program (QPP) takes a comprehensive approach to payment, which rewards value and outcomes in one of two ways: Merit-based Incentive Payment System (MIPS) and Advanced Alternative Payment Models (APMs). Instead of basing payment only on a series of billing codes, the Quality Payment Program adds consideration of quality through a set of evidenced-based measures that were primarily developed by clinicians.